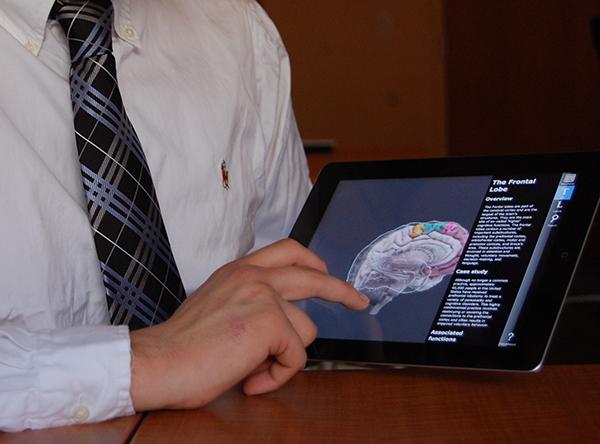
Next year’s new GW medical students will have made it through one of the most selective admissions processes in the country. But they’ll each get a bonus: a new iPad.
The School of Medicine and Health Sciences will distribute iPads to its about 180-student first-year class for the first time next fall, joining a host of medical schools that are investing in a tool that is becoming more prevalent for doctors around the country.
“They’ll get their white coats and their iPads and they’ll be new GW medical students,” said Jeffrey Akman, dean of the medical school, at a recent Faculty Senate meeting.
The iPads will complement a new curriculum that cuts down on basic science classes taken in the first two years to “get students into the clinics and hospitals more rapidly,” Akman said. The school will also reduce lecture time and stress team-based learning.
“It’s about continuing to emphasize areas as we look toward what a physician of next generation should look like in terms of training,” he added.
Purchasing iPads for each member of the first-year class could rack up to nearly $70,000, but Bernhard Wiedermann, a professor of pediatrics who is leading the curriculum revision, said the school will likely receive an educational discount. She added that the school plans to cover the cost with money from school’s academic fundraising White Coat Initiative.
Howard Lee, a fourth-year student, said the iPads are a good investment for budding doctors. He bought one in his second year because it seemed more practical for note taking, textbooks and filing information on patients.
“You can do two things at once, so sometimes if you’re listening to an audio recording of your lecture you can look at your notes at the same time,” Lee said, adding that he sometimes watches videos of procedures before heading to class.
He added that tablets are better for medical students than laptops because they can use them easily when moving into clinical education in the third and fourth year.
Younger doctors around the country use iPads or tablets in patient rooms – analyzing patient symptoms and health history through statistical software that can be downloaded apps. Using iPads can improve efficiency, allowing doctors to enter information more quickly, a University of Chicago study found last year.
Wiedermann said the school expects having iPads will streamline communications between students and faculty. Students will have direct access to 3-D anatomical models, databases and medical journals.
Current students praised the program’s switch to a paperless curriculum for practical and environmental reasons. Other programs at the University of Arizona, Case Western Reserve University and the University of Virginia have made the same move in the past few years.
Stanford University gave first-year medical students iPads until this year, when they started giving students a stipend with which they could purchase any tablet.
Jessica Price, a fourth-year student interested in family medicine, said students will be able to access a number of medical applications on the iPad in class, which can add to the classroom experience. Some schools, including Stanford, recommend apps that can show how different regions of the brain function or simulate reading CT scans.
She added that a paperless curriculum will attract students looking for the latest technology.
“People would see that as being a program and a school that’s moving forward in terms of what technology they’re using and being on the front edge of having students take advantage of resources available,” she said.
The medical school’s 2.1 percent acceptance rate was already the most selective in the country last year, despite its research rank only reaching No. 57, according to U.S. News & World Report.
The curriculum will also make use of a patient simulation center – where students learn to talk to patients about sensitive subjects like death and sexual history – that will open in Ross Hall this spring.
The revised curriculum will also have students working in clinics nearly 6 months sooner into their medical education than they do now. Wiedermann said the technology will “transform education.”
“Students working on a class project could develop instructional videos for patients with a particular illness, demonstrating both their knowledge of a disease process and creating new knowledge that improves health care,” he said.